Rosacea is a skin condition that causes facial flushing and visible blood vessels. It might also produce tiny, pus-filled pimples. These signals and symptoms may flare up for weeks to months before dissipating again. Rosacea can be mistaken for acne or other skin concerns.
Rosacea affects men and women of all races, but it is most common among middle-aged white females. Rosacea has no cure; nevertheless, it may be treated to minimize and control the symptoms.
Types of Rosacea
Rosacea has four distinct types, although many people experience symptoms from more than one type.
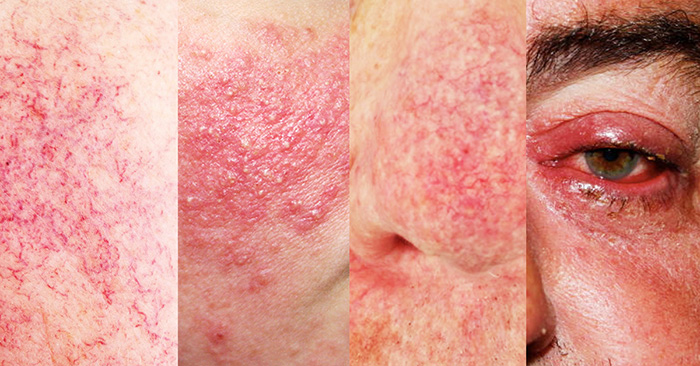
Erythematotelangiectatic Rosacea
Erythematotelangiectatic rosacea is marked by persistent redness on the face. Small blood vessels beneath the skin’s surface may grow enlarged and visible; these symptoms frequently flare up and then fade away. The redness can get more severe, cover more skin, and even become long-lasting without treatment.
Papulopustular Rosacea
In papulopustular rosacea, “whitehead” pustules and red, inflammatory papules are common. These typically show up on the cheeks, jawline, and forehead and are frequently mistaken for acne.
Facial redness and flushing are other symptoms. Severe papulopustular rosacea can produce up to 40 blemishes that take a long time to heal. Blemishes may also appear on the scalp, neck, or chest.
Phymatous Rosacea
Phymatous rosacea causes the skin to thicken and scar, resulting in bumps, puffiness, and color changes. This uncommon yet treatable condition most often affects the nose, resulting in rhinophyma or a bulbous nose. Phymatous rosacea appears more frequently in males than females.
Ocular Rosacea
The eyes of someone with ocular rosacea may appear watery or bloodshot. There may also be an uncomfortable sensation in the eyes. Ocular rosacea can produce chronically dry, sensitive eyes, and cysts may develop on the eyelids.
Potential Causes of Rosacea
Although the underlying cause of rosacea remains unknown, recent research has revealed key elements of the disease process that might lead to significant improvements in treatment.
According to numerous studies, facial redness is most likely to be the start of an inflammatory continuum induced by a combination of neurovascular diseases and the innate immune system.
In addition to neurovascular diseases and the immune response, Demodex folliculorum, a microscopic mite that lives on the skin, has long been linked to rosacea. This bug is a typical resident of human skin, but it has been discovered to be considerably more prevalent in patients with rosacea. Furthermore, two genetic variants in the human genome may be associated with rosacea.
Recent studies have linked rosacea to an increased risk of a growing number of potentially serious systemic diseases, suggesting that rosacea may be a consequence of systemic inflammation.
Topical Ivermectin for Rosacea Inflammatory Lesions
Ivermectin 1% cream is a topical prescription medication indicated for the treatment of inflammatory lesions in papulopustular rosacea. This is different from oral ivermectin treatment for other diseases like scabies or parasite infections.
Its mechanism of action is unknown, but it may be due to a combination of anti-inflammatory effects and antiparasitic actions on the Demodex mite, which lives on the skin and may contribute to rosacea.
Demodex mites are present in greater quantities in individuals who have rosacea. 35-50% of persons with rosacea had more Demodex mites on their facial skin symptoms. The mites enter the hair follicles and sebaceous glands, causing inflammation.
Demodex mites induce damage to the epithelium, the top layers of skin. They also cause the skin to become hypersensitive. Rosacea patients are also more sensitive to UV radiation than other people. The result is papules and pustules formation.
Topical ivermectin enters the pilosebaceous units and destroys the Demodex mites, reducing inflammatory lesions of rosacea as a consequence.
Other Topical Treatment for Rosacea
At the start of therapy, a combination of topical and oral medicines may be suggested. These medications can help to relieve facial redness and discomfort, as well as reduce blemishes.
After symptoms have been controlled, many individuals choose to utilize only topical treatments. The following topical treatments may be prescribed by your doctor:
- Metronidazole or other antibiotic preparation
- Retinoids
- Azelaic acid gel
- Brimonidine
Effectiveness of Topical Ivermectin 1% Cream
In 2016 two randomized, double-blinded studies by Leah A Cardwell, et al., “New developments in the treatment of rosacea—role of once-daily ivermectin cream”, ivermectin 1% cream applied once daily was found to be more effective than vehicle control in the treatment of papulopustular rosacea.
Based on The Investigator’s Global Assessment of Rosacea Severity (IGA-RS), after the 12-week period, participants using ivermectin 1% cream were evaluated as “clear” or “nearly clear” at 38.4% and 40.1% for study 1 and study 2, respectively. The vehicle control group was evaluated as “clear” or “nearly clear” at 11.6% and 18.8% for study 1 and study 2, respectively.
In another 52-week investigator-blinded, randomized, parallel-group study, the efficacy of ivermectin 1% cream was superior to metronidazole 0.75% cream in the treatment of inflammatory lesions in papulopustular rosacea.
After the 52-week period, from baseline, ivermectin 1% cream reduced inflammatory lesions by 83.0%, whereas metronidazole 0.75% cream reduced them by 73.7%.
Additionally, participants using ivermectin 1% cream were rated as “clear” or “nearly clear” at 84.9% while participants using metronidazole 0.75% cream were rated as “clear or “nearly clear” at 75.4%.
Adverse Effect of Skin Irritation
Burning or stinging of the skin was the most typical adverse effect, which occurred in less than 1% of patients in clinical trials. The skin may feel dry, itchy, or irritated.
The occurrence of adverse effects is comparable with that observed with metronidazole cream and azelaic acid cream.
Because there have been no studies conducted on pregnant or breastfeeding women, it’s not advised for them.
How to Use Ivermectin 1% Cream
After cleansing and drying your face, apply a thin layer to the entire face once daily.
Avoid the inside of the nose or mouth, and eyes. Before applying any additional rosacea treatments, makeup, or sunscreen, allow the cream to dry on your face. After using it, wash your hands carefully.
It’s possible that your rosacea will get worse for the first week or two of usage. This is due to the fact that, at first, the dead and decaying Dermodex mites cause an increase in skin irritation.
Thereafter, however, things should improve gradually. There’s a chance that your skin won’t tolerate ivermectin 1% cream for a long time – it might make rosacea worse – but this is uncommon.
Conclusion
Ivermectin 1% cream has been shown to be effective for the treatment of moderate to severe papulopustular rosacea by reducing the inflammatory lesions. It has the combination of anti-inflammatory effects and antiparasitic actions on the Demodex mite, which has been linked to rosacea.
For those who have difficulties treating inflammatory lesions of rosacea with other topical agents, topical ivermectin cream may be worth considering as an option. Consult with your doctor regarding whether ivermectin 1% cream is appropriate for you.

